Lymphatic Filariasis
The cause to the illness
Human lymphatic filariasis (GCBH) is caused by three species: Wuchereria bancrofti (W.bancrofti), Brugia malayi (B.malayi), Brugia timori (B.timori).
In Vietnam, two species of Lymphatic filariasis have been discovered so far are W
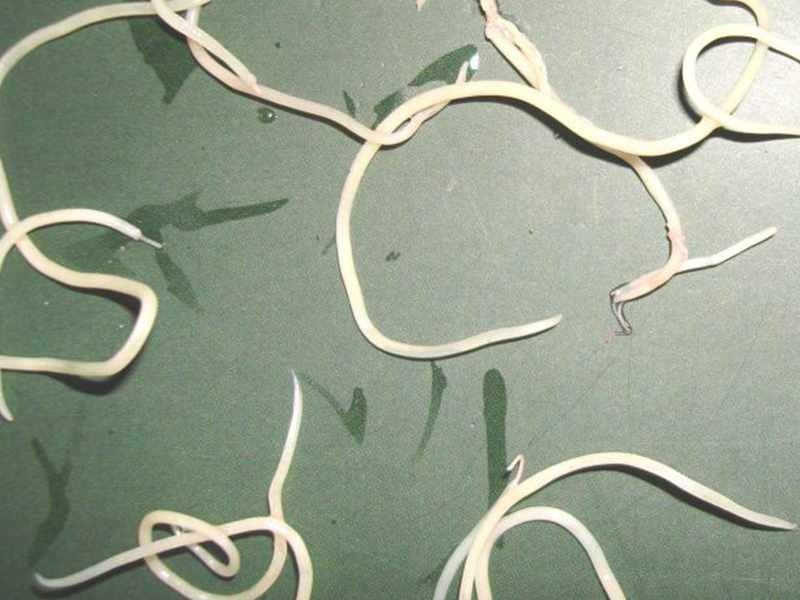 .ancrofti have been discovered.
.ancrofti have been discovered.The development cycle of lymphatic filariasis
Wuchereria bancrofti development cycle (W.bancrofti)
1) When mosquitoes have worm larvae, they only mediate to suck human blood.
2) Larvae to the lymphatic system develop into adult worms and live in the lymphatic system of humans.
3) Adult female worms produce larvae, which circulate in the blood and usually appear in peripheral blood at night (8 pm to 4 am)
4-5-6-7) Mosquitoes suck blood from the filariasis larvae into the stomach of the mosquito, through the stomach wall, and then transfer to the mosquito chest muscle. Here the larvae develop through three stages (L1-L3) to become infectious larvae. The time from larvae into the body of mosquitoes until larvae cause infection is about 10-14 days.
8) Infected larvae move to the mosquito nets and spread to others when they suck blood.
 .
.Life expectancy GCBH mature from 4-6 years, larvae in the blood to 1 year.
Situation of infection with lymphatic filariasis
In the world: worm disease is very common in tropical countries. Worldwide, 120 million people in 73 countries are infected and about 1.1 billion people (about 20% of the population) live in endemic areas
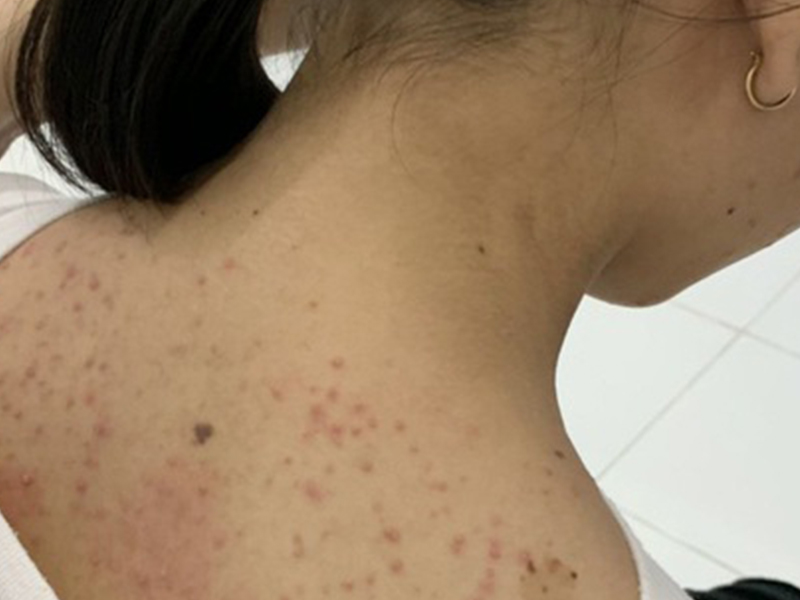
Common complications are elephant's foot edema, urinary support. He greatly affects the labor, aesthetics and life of the patient.
In Vietnam: according to survey data before 2000, worms were distributed mainly in Northern Vietnam. The disease is common in provinces in the Red River Delta, especially in 5 provinces: Hai Duong, Hung Yen, Thai Binh, Ha Nam and Nam Dinh. The overall infection rate is 2.01%
Survey results from 2000-2005 nationwide showed that worm disease was only widely distributed in 12 districts in 7 provinces: Hung Yen, Thai Binh, Hoa Binh, Quang Binh, Khanh Hoa, Ninh Thuan with infection rates from 0.
 .3 -13%.
.3 -13%.Harms and symptoms of the disease:
Common complications are elephant's foot edema, urinary support He greatly affects the labor, aesthetics and life of the patient.
The majority of patients (90-95%) are infected with lymphatic filariasis (have larvae in the blood) but have no clinical manifestations for years or possibly a lifetime. In the case of clinical manifestations, there may be different symptoms. Common are:
1. Acute symptoms:
Fever: high fever, often presenting suddenly; Accompanied by fatigue and numerous headaches; often recurrent episodes; Each session usually lasts from 3-7 days.
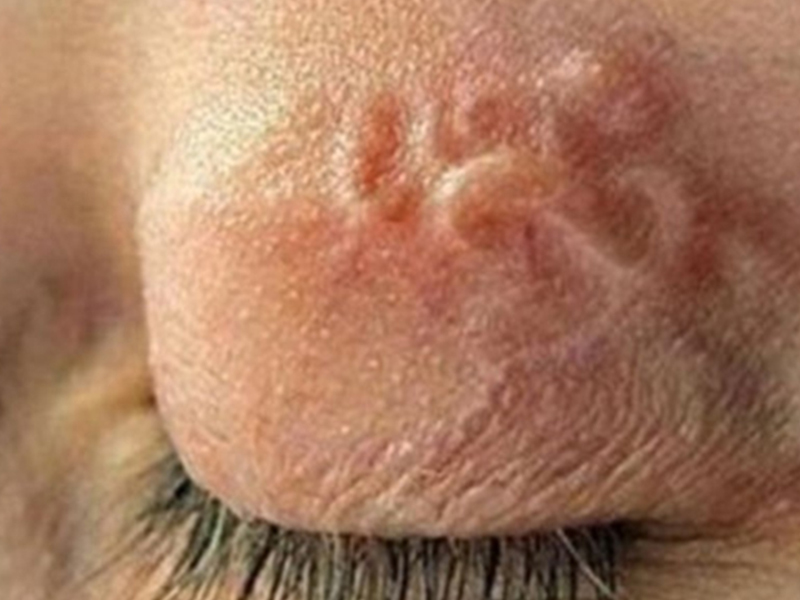
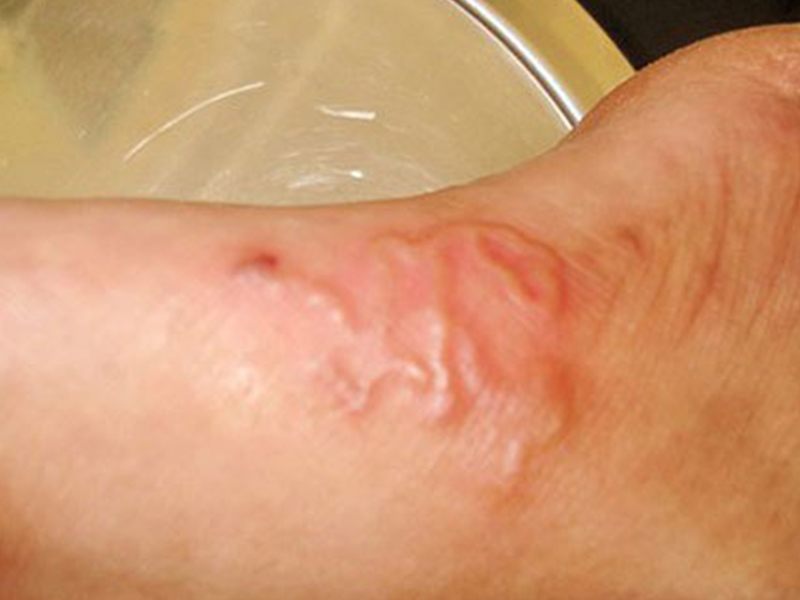
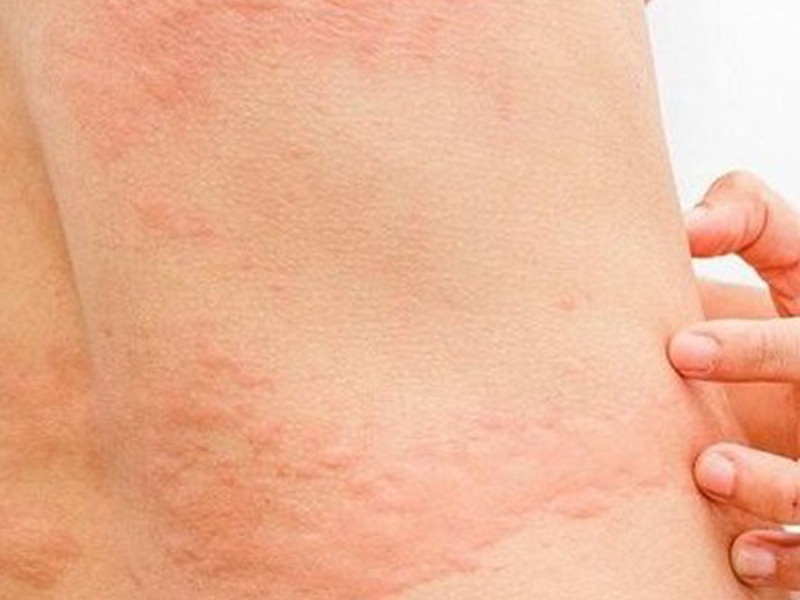
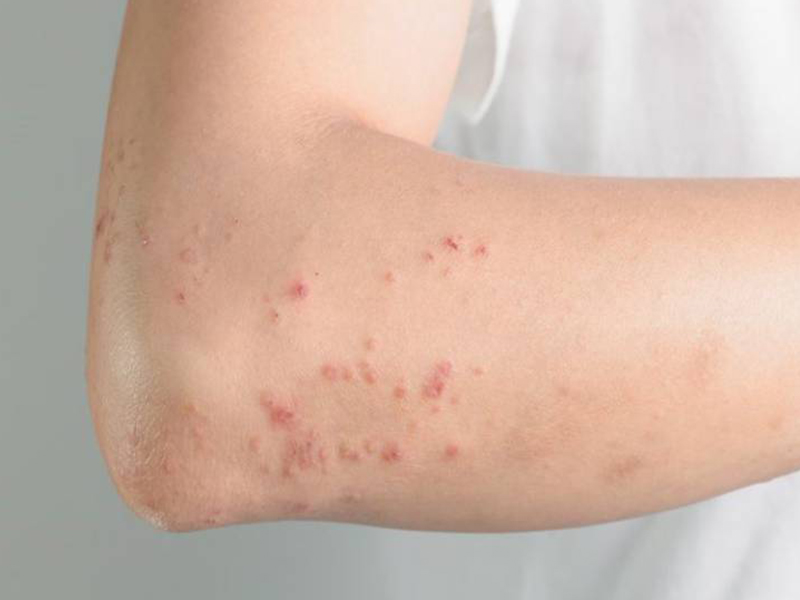
Lymphadenitis and lymphadenitis: usually occurs after a few days of fever. Inflammatory red lines, accompanied by painful symptoms, run along the lymphatic vessels, usually the inner surface of the lower extremities. Inguinal lymph nodes can be swollen, painful.
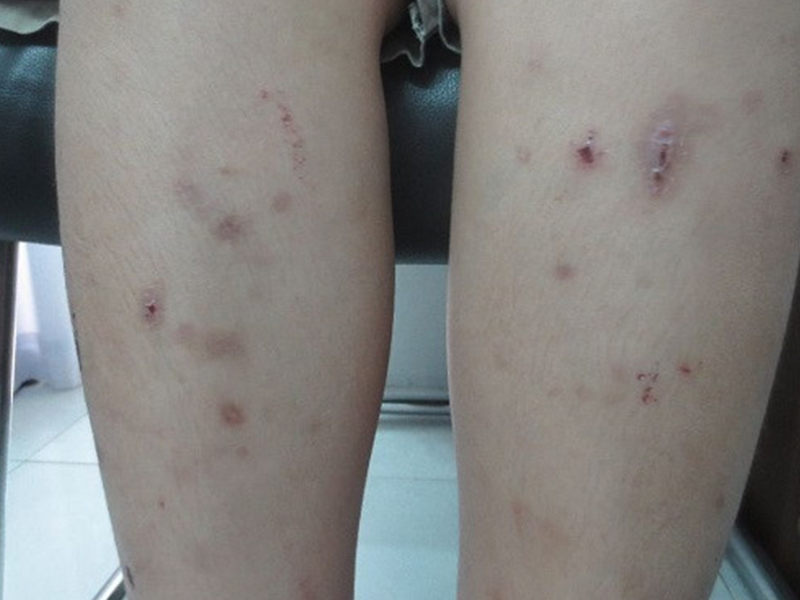
2. Common chronic symptoms:
Inflammation or swelling of the genitals such as inflamed testicles, testes, hydroceles In case of chronic genital inflammation in the genitals, can cause symptoms of elephant scrotum or elephant breast.
Edema of the lower extremities: is a consequence of chronic inflammation of the lymph nodes and lymphatic vessels of the lower extremities, characterized by stiff, thickened legs. Depending on the level, edema may occur from the bottom of the foot to the thigh.
Elephant foot edema caused by lymphatic worms
Nursing accept: urine is opaque white like rice bran water, for a long time does not settle, sometimes bloody. Where the amount of nutrients in urine is much, so long as the urine can be frozen.
Diagnose:
Definitive diagnosis: the most common and simplest method today is to detect larvae in peripheral blood: conduct peripheral blood collection at night (from 20 hours to 24 hours), take it as a sample, giemsa staining and microscopic examination of larvae. However, in cases of elephant foot edema or nourishment, the rate of detection of larvae in the blood is very low (only about 3-5% of patients)
For B.malayi: take peripheral blood at night (from 20 hours to 24 hours), then make the specimen, take the dye staining and detect larvae under the microscope.
 .
.For W.bancrofti: in addition to the method of nocturnal blood testing, it is now possible to detect rapidly by the ICT rapid immuno-diagnostic test (immuno-chromatographic test), which can perform blood tests during the day.
Preventive measures:
Treatment of the whole population with GCBH infection rate of 1% or more and treatment of cases in scattered infection.
Kill mosquitoes and sleep nets to avoid mosquito bites.
KTV. KHONG VY . Dịch vụ: Thiết kế website, quảng cáo google, đăng ký website bộ công thương uy tín
Related news
-
 Parasitical Worms.com Tests to find the cause of urticaria, diagnosis of urticaria results will be available throughout the day. After the results the doctor will explain, point out the abnormal signs for your child to understand and he will prescribe medication for home. Question Hello doctor: I ...
Parasitical Worms.com Tests to find the cause of urticaria, diagnosis of urticaria results will be available throughout the day. After the results the doctor will explain, point out the abnormal signs for your child to understand and he will prescribe medication for home. Question Hello doctor: I ... Parasitical Worms.com Adult flukes are very small, 3 - 6 mm long, with 4 suction heads and a double hook, very short neck; coal consists of 3 segments, the final flukes have several hundred eggs, size 45 x 35 mcm, very similar to Toenia spp eggs. The disease is caused by the larva Echinococcus ...
Parasitical Worms.com Adult flukes are very small, 3 - 6 mm long, with 4 suction heads and a double hook, very short neck; coal consists of 3 segments, the final flukes have several hundred eggs, size 45 x 35 mcm, very similar to Toenia spp eggs. The disease is caused by the larva Echinococcus ... Parasitical Worms.com Some diseases caused by larvae of the anisakinae family parasitize marine mammals. In humans, the parasite falls into a dead-end, or severe or severe illness depending on the place of parasite, number of larvae and tissue responses. Diagnosis is often difficult and the most ...
Parasitical Worms.com Some diseases caused by larvae of the anisakinae family parasitize marine mammals. In humans, the parasite falls into a dead-end, or severe or severe illness depending on the place of parasite, number of larvae and tissue responses. Diagnosis is often difficult and the most ... Parasitical Worms.com Illness caused by the nematode of Angiostrongylus cantonensis parasitizes and causes disease in the meninges, invasion of the brain can lead to death. Commonly called Meningitis - brain caused by Angiostrongylus cantonensis. The causative agent of nematode ...
Parasitical Worms.com Illness caused by the nematode of Angiostrongylus cantonensis parasitizes and causes disease in the meninges, invasion of the brain can lead to death. Commonly called Meningitis - brain caused by Angiostrongylus cantonensis. The causative agent of nematode ... Fascioliasis is two types of fascioliasis and small liver fluke. People are infected with food, skin. Flukes can cause hepatitis, liver tumors, liver necrosis, but fortunately, liver fluke can be cured if detected early, treated in a reputable facility with a good doctor, using drugs. Good, ...
Fascioliasis is two types of fascioliasis and small liver fluke. People are infected with food, skin. Flukes can cause hepatitis, liver tumors, liver necrosis, but fortunately, liver fluke can be cured if detected early, treated in a reputable facility with a good doctor, using drugs. Good, ... Parasitical Worms.com Diagnosis is determined by seeing sparganum larvae from the wound. Clinical and prehistoric images of frog meat, eye-copying as well as the habit of eating undercooked snakes, mice, and eels are important factors for diagnosis. Doctor: Le Thi Huong Giang Medical Consultation: ...
Parasitical Worms.com Diagnosis is determined by seeing sparganum larvae from the wound. Clinical and prehistoric images of frog meat, eye-copying as well as the habit of eating undercooked snakes, mice, and eels are important factors for diagnosis. Doctor: Le Thi Huong Giang Medical Consultation: ... MUSHROOM DISEASE (Aspergillus) 1. Epidemiology. Aspergillus fungus is one of the largest fungal strains, present in all over the world, there are about 100 species, currently there are about 20-30 species that cause disease in humans, important strains are A. fumigatus, A. flavus , A. niger such as ...
MUSHROOM DISEASE (Aspergillus) 1. Epidemiology. Aspergillus fungus is one of the largest fungal strains, present in all over the world, there are about 100 species, currently there are about 20-30 species that cause disease in humans, important strains are A. fumigatus, A. flavus , A. niger such as ... MUSHROOM DISEASE Cryptococcosis (Tolurosis, European Blastomycois) 1. Etiology and epidemiology Cryptococcosis is also known as the European Blastomycose mycosis caused by Cryptoccocus neoformans, a thick cystic yeast, has serotypes A, D (C. neoformans var. Neoformans) and B, C ( C.neoformans var. ...
MUSHROOM DISEASE Cryptococcosis (Tolurosis, European Blastomycois) 1. Etiology and epidemiology Cryptococcosis is also known as the European Blastomycose mycosis caused by Cryptoccocus neoformans, a thick cystic yeast, has serotypes A, D (C. neoformans var. Neoformans) and B, C ( C.neoformans var. ... MUSHROOM DISEASE Sporotrichosis (Gardener Disease) 1. Epidemiology and etiology Sporotrichosis is a chronic disease caused by Sporothrix schenckii that causes damage to the skin or internal organs (also known as gardener disease - gardener's disease). This is a dimorphic mushroom. In nature, ...
MUSHROOM DISEASE Sporotrichosis (Gardener Disease) 1. Epidemiology and etiology Sporotrichosis is a chronic disease caused by Sporothrix schenckii that causes damage to the skin or internal organs (also known as gardener disease - gardener's disease). This is a dimorphic mushroom. In nature, ... CANDIDA MUSHROOM 1. Germs Candidiasis is an acute, subacute or chronic disease caused by Candida-like yeasts, mostly Candida albicans. Candidiasis is available in the body (bronchus, oral cavity, intestine, vagina, skin around the anus) normally in non-pathogenic form. When having favorable ...
CANDIDA MUSHROOM 1. Germs Candidiasis is an acute, subacute or chronic disease caused by Candida-like yeasts, mostly Candida albicans. Candidiasis is available in the body (bronchus, oral cavity, intestine, vagina, skin around the anus) normally in non-pathogenic form. When having favorable ...